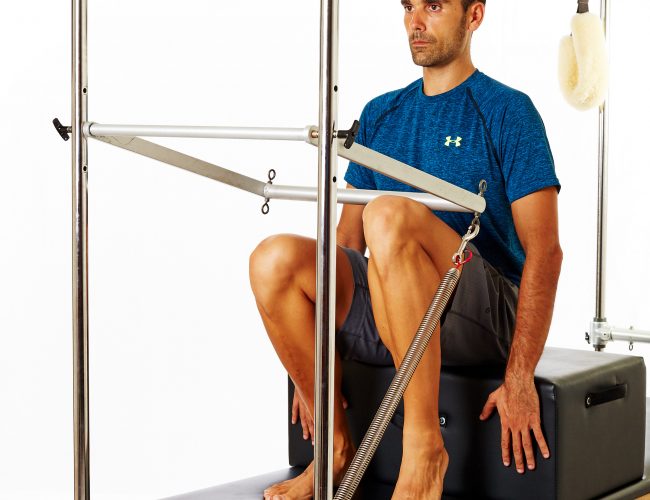
Osteoporosis treatment and exercise
Thu,Aug 10, 2017 at 12:56PM by Carla Mullins
Osteoporosis treatment and exercise is a mantra of doctors, physiotherapists and rehabilitation practitioners worldwide, however it can be a little overwhelming to understand what this actually means. How does this translate into reality for many people? What is proven to be effective and what is actually a fad?
In this article we explore osteoporosis and how it is diagnosed, how it is characterised and the guidelines as to what is appropriate for treatment. Some of the information we have gathered for this article has come from recent training with Monique Kurki (musculoskeletal physiotherapist and certified pilates instructor with a special interest in this area, as well as from our own literature reviews conducted for our training courses for movement professionals. The purpose of this article is about understanding what to do and how to work with people once diagnosed with osteoporosis or osteopenia, however it is not about the prevention of osteoporosis.
What is osteoporosis?
Osteoporosis is a disease characterised by low bone mass and micro-architectural deterioration of bone tissue, leading to bone fragility and increased fracture risk5. However, for epidemiological and clinical purposes, osteoporosis (for post-menopausal women only) is defined by a Bone Mineral Density test result (generally of hip and spine). When a person is given their test result they will see a T score and a Z score. The T score is a measure with an average level of bone mineral density of 2.5. When measured on a bell curve if somebody has a certain level of deviation from the mean, then they are considered to be osteopenic or osteoporotic. The degree of difference will be marked and the label applied on the test results. A person will also be given a Z score which compares their score to what would be expected of someone of equivalent age, gender and race. These measures are then used to identify if a person is at risk of bone fractures.
Osteopenia is the term used by doctors to describe low bone density. People with osteopenia have bones that are weaker than normal, but not weak enough to be called osteoporosis. Nguyen et al (1993) stated “Bone mass, assessed by Bone Mineral Density (BMD), is a good predictor of fracture risk, with each standard deviation (SD) decrease in BMD being associated with at least a twofold increase in the risk of fracture”7.
Who is affected by osteoporosis?
In Australia:
// One in two women over the age of 50 and one in four men have low bone density with a prediction of fracture in their lifetime
// More than 50% of women and 70% of men who sustain a low trauma fragility fracture (eg. fall from a standing height) have a diagnosis of osteopenia rather than osteoporosis
In other words, its prevalence is such that there is a high likelihood that you will see someone who has either been diagnosed with or is at risk of having osteopenia or osteoporosis.
Overall fracture risk from osteoporosis
Fracture risk however, is a function of BOTH trauma sustained (eg. falls) and bone strength (which in turn depends on both the quantity of bone (mass) and its architecture). Half of all falls occur around the home and approximately one third of people over 65 fall each year. It is estimated around 6% of falls result in a fracture, so preventing falls has become an important part of managing bone health and osteoporosis treatment.
Falls are most commonly caused by:
// Poor muscle strength, especially of legs (and also poor flexibility)
// Problems with balance due to weak muscles, slow reflexes, low blood pressure, inner ear problems, some medicines, poor nutrition (also feet and shoe issues)
// Poor vision
// Home hazards that cause tripping
Physiology of bone and bone mineral density
Bone is constantly remodelling; microscopic amounts of bone tissue in the skeleton are removed by osteoclasts (bone resorption) and then replaced with new tissue by osteoblasts (bone formation). In the first year of life, almost 100% of the skeleton is replaced, whilst in adults, remodelling proceeds at about 10% per year. Remodelling occurs following injuries like fractures, but also occurs in response to the functional demands of mechanical loading.
Bone mineral density is reduced when the rate of bone resorption is greater than the rate of bone formation, resulting in a net bone loss of both trabecular and cortical bone. Many factors can contribute to bone resorption outpacing bone formation.
Osteoporosis and osteopenia can be found in the younger population (ie under 65)
Whilst age is a significant factor in the existence of osteoporosis, there are some people that can be susceptible to early onset osteoporosis. Those people include:
// Those who have been using steroids for more than 5 years – think of asthmatics or people with chronic illness like multiple sclerosis
// Cancer patients who have been through chemotherapy
// Women who have had early onset menopause
// People who have had any one of a number of autoimmune diseases that can affect the absorption of vitamin D or nutrients
Don’t always assume that your younger clients will not be at risk of osteoporosis and therefore won’t require osteoporosis treatment. Rather, make sure that you do a thorough screening and questionnaire with them to ensure that you are able to adequately determine if there is the potential for risk. In those cases I always suggest that they consult their doctor for testing.
Osteoporosis treatment and exercise – how can pilates help?
In Australia many of the guidelines on working with people with osteoporosis are detailed in the 2017 Beck BR, et al. Exercise and Sports Science Australia (ESSA) position statement on exercise prescription for the prevention and management of osteoporosis. J Sci Med Sport (2016), http://dx.doi.org/10.1016/j.jsams.2016.10.001. Those guidelines give details about:
// Balance
// Joint mobility
// Load or resistance levels
and what are the appropriate testing and levels for those people with osteoporosis and osteopenia at different risk levels, categorised from low risk to high risk.
Balance for osteoporosis treatment in a pilates studio setting
Specific balance work should include focus on challenging all parts of the balance system, namely proprioceptive, vestibular and visual. To be honest this should be part of any movement class regardless of the person’s age or bone health. Maintaining good balance and fall prevention is an essential part of a functional life. Accordingly, a good movement class will incorporate various techniques to challenge the balance systems and build reaction times in order to help people recover from a fall. There has been research coming out of the University of Queensland’s Physiotherapy Department about how balance starts to decline in women in their 40s. Some ideas for working with balance in a pilates class include:
Reformer Step up (from Reformer Three resource manual)
Moon walking in the baby arc (from our Cancer and Exercise book)
Bird on the CoreAlign (from CoreAlign 1 Vertical Axis Manual)
Joint mobility
Working on maintaining dorsiflexion in the feet and hips is another great way to improve someones balance and gait which can reduce falls risk. Below is an example of how you can use the HedgeHogs as a way to help improve dorsiflexion in the ankles.
Hedgehog Talus Glide video
Bottom loaded legs on the Trapeze Table (from our Trapeze Table resource manual)
Adding some level of load
Whilst pilates may not involve the high loads that you will see in weight lifting, we can add load if we think about smart use of the apparatus. I like to use the Trapeze Table and Bottom Loaded Push Through Bar, with variations in the springs to ensure to increase loaded work in the studio. I particularly like to work this way for people who feel uncomfortable with a free bar or in a gym setting. In this setting we can help improve technique and gradual load to create what is referred to as the osteogenic response in bones. It is important to remember that there are different levels of impact loading for people undergoing osteoporosis treatment, dependent on their risk levels. At Body Organics we rely on the standards detailed by ESSA based on the Beck et al. Journal of Science and Medicine in Sport, May 2017 to determine appropriate loading levels when working with clients with different risk ratings.

Trapeze Table bottom loaded lunges

Trapeze table bottom loaded deadlifts
There are contraindications for people with osteoporosis and those contraindications include avoiding loaded flexion, eg spine stretch on the Reformer or Tower on the Trapeze Table. All of these contraindications are detailed in our Body Organics repertoire manuals, including our Trapeze Table (Cadillac) resource manual.
To learn more about osteoporosis, its causes, osteoporosis treatment and well as prevention and living with the condition, visit the Osteoporosis Australia web site.
References for osteoporosis treatment and exercise
1. http://www.who.int/chp/topics/Osteoporosis.pdf
2. http://www.osteoporosis.org.au/sites/default/files/files/ Consumer%20Guide%202nd%20Edition.pdf
3. http://whqlibdoc.who.int/trs/WHO_TRS_921.pdf
4. http://www.who.int/chp/topics/Osteoporosis.pdf (written 2004)
5. Clinical practice guideline for the prevention and treatment of osteoporosis in postmenopausal women and older men. http://www.racgp.org.au/your-practice/guidelines/ musculoskeletal/osteoporosis/ Melbourne: RACGP, 2010
6. http://www.who.int/chp/topics/Osteoporosis.pdf
7. Nguyen TV, Sambrook PN, Kelly PJ, et al. Prediction of osteoporotic fractures by postural instability and bone density.BMJ1993; 307: 1111-1115
8. www.osteoporosis.org.au/exercise
9. Nguyen T, Center J, Eisman J. Osteoporosis: underrated, underdiagnosed and undertreated. Medical Journal of Australia 2004;180(5 Suppl):S18–22
10. http://www.osteoporosis.org.au/about-osteoporosis
11. http://www.racgp.org.au/your-practice/guidelines/redbook/ osteoporosis/
12. www.arthritiswa.org.au
13. Building healthy bones throughout life-An evidenceinformed strategy to prevent osteoporosis in Australia” Ebeling et al (2013) arising from the 2011 Osteoporosis summit held in Sydney) https://www.mja.com.au/sites/default/files/ issues/002_01_040213/MJA%20OpenSupplement.pdf
14. Interaction between Muscle and Bone- Hiroshi Kaji J Bone Metab. 2014 Feb; 21(1): 29–40. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3970293/
 0
0